Pathophysiology and Management part 1
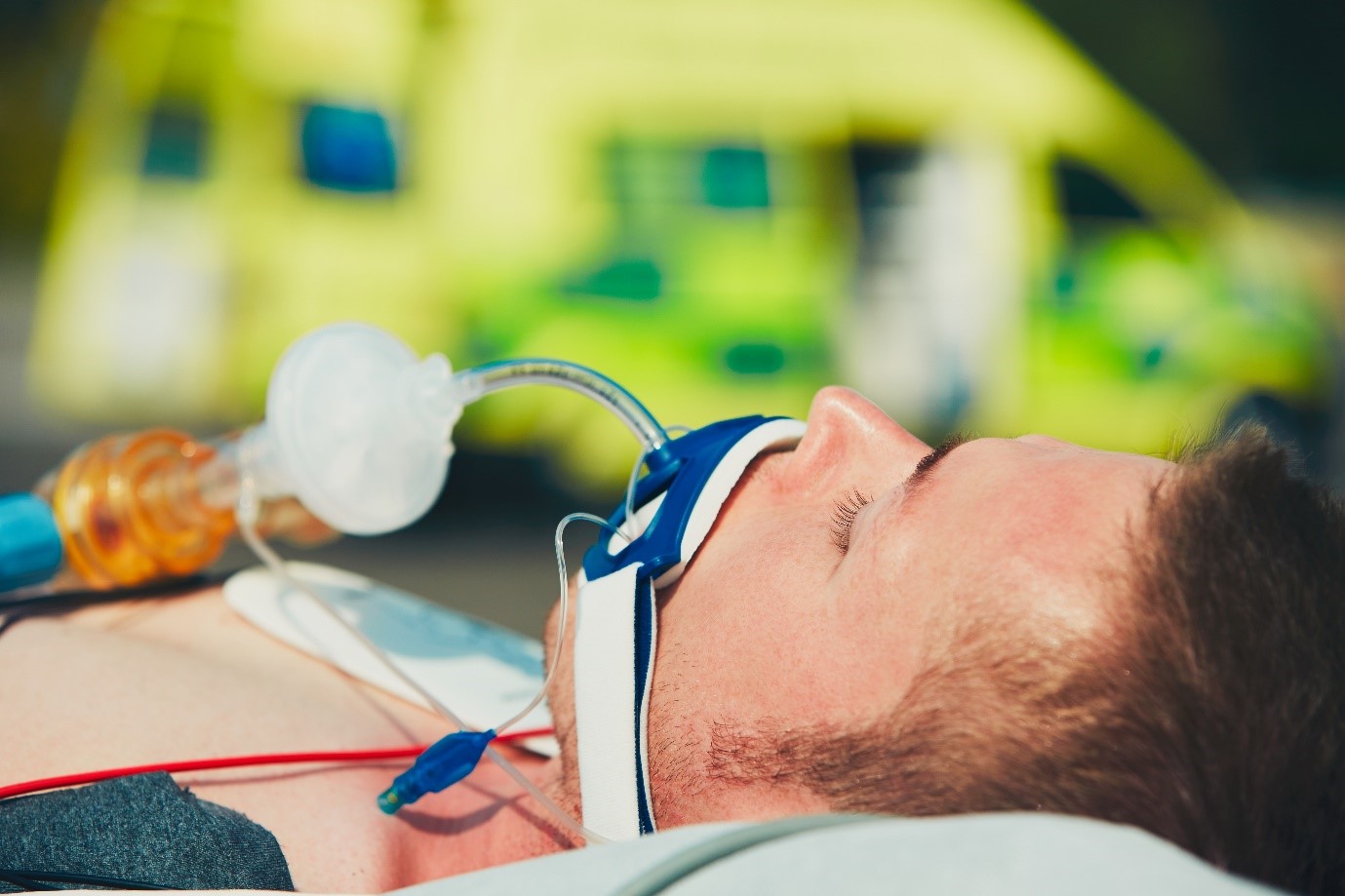 A patients’ breathing can be affected by several medical and traumatic events. The overall aim is to ensure that the patient has adequate and effective respirations/ventilations. This may be done through assisting or mechanically ventilating, or through drug treatment.
A patients’ breathing can be affected by several medical and traumatic events. The overall aim is to ensure that the patient has adequate and effective respirations/ventilations. This may be done through assisting or mechanically ventilating, or through drug treatment.
Respiratory arrest – For several medical or traumatic reasons, a patient may be in respiratory arrest. This is where the patient is making no respiratory effort, and no air is entering or exiting the lungs. A Bag Valve Mask (BVM) is needed to ventilate the patient. Follow a stepwise airway approach to ensure that the patient is getting adequate and effective ventilations. Ventilate the patient at a rate of 10 ventilations per minute, or a ventilation every 6 seconds. Be wary of the volume of ventilation when ventilating a patient with a BVM, over-ventilating the patient or being heavy handed with the BVM could cause potential barotrauma of the lungs.
Respiratory distress – Some medical or traumatic cases may cause a patients’ respiratory rate to be too high or too low, affecting their ability to ventilate their lungs adequately and effectively. If your clinical judgement feels that this respiratory effort is ineffective, then you may need to support the patients’ breathing with a BVM.
SPO2 – In some cases, a patients’ SPO2 may be low due to the medical or traumatic event ongoing. Supplemental Oxygen may be required via a face mask to support and normalise their SPO2 levels. Clinical judgement is required as per what face mask is used and how much is applied to reach the desired SPO2. In cases of major/critical trauma, patients should receive 100% Oxygen via facemask. This is to help alleviate some of the negative processes that occur in a patient with critical traumatic injuries.
Oedema – In some events, fluid/oedema may collect in the lungs creating a barrier between the air and the walls of the alveoli. This makes gaseous exchange difficult as the Oxygen and Carbon dioxide must try and diffuse through the fluid to reach the cell membranes. The presence of oedema is usually indicated through auscultated crackles, frothed sputum, or an audible ‘bubbling’ on the chest. Patient positioning can help alleviate the immediate difficulty in breathing by oedema through sitting them up in an upright position. Further treatments, such as medications, may be required to provide greater support to the patients’ breathing.
Asthma – An inflammatory disease of the airways associated with episodes of reversible over-reactivity of the airway smooth muscle. Asthma can range from mild to life-threatening, and usually requires medication to treat. Within the UK, nebulised Salbutamol is initially administered to ease the effects. If this fails, then nebulised Ipratropium Bromide is also administered. In severe cases, hydrocortisone can also be administered. In life-threatening asthma, failing nebulisation, Adrenaline 1:1000 IM can be administered, followed by Hydrocortisone. If respiration fails, then supportive means via BVM may be required whilst rapidly transporting to hospital.